Many of us do not have to worry about our body suffering from prolonged exposure to the stress hormone, cortisol. But what happens to us when we do? How do we know that we are suffering from Cushing’s syndrome? And when should you get a urologist’s opinion and advice? The following information should help answer these questions.
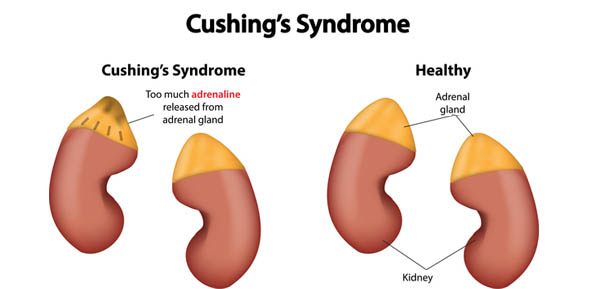
What happens under normal conditions?
The adrenal glands are endocrine glands that are located on the top of both kidneys. Each adrenal gland is composed of two layers, an inner layer known as the medulla and an outer layer known as the cortex. Normally, the adrenal cortex secretes a variety of steroid hormones including cortisol, which helps the body respond to stress and change. It also regulates salt and water levels that affect blood volume and blood pressure. The secretion of cortisol is regulated by the pituitary gland, which is located inside the head at the base of the brain. Chemical signals from the pituitary are carried by the bloodstream and act on the cells of the adrenal cortex to promote the secretion of cortisol. This chemical messenger is called corticotrophin or adrenocorticotropic hormone (ACTH). When needed, ACTH is secreted by the pituitary and, as a result, cortisol is then secreted into the circulation. When cortisol is no longer required, the high levels of cortisol in the blood are detected by the pituitary. This feedback causes the pituitary to reduce ACTH secretion so that cortisol levels are reduced. The overall system acts like a thermostat and is highly regulated.
What is Cushing’s syndrome?
Cushing’s syndrome (CS) occurs when there is excessive production of cortisol that is not controlled by the normal regulatory system. It can also be caused by excessive or prolonged use of steroids.
What causes Cushing’s syndrome?
Cushing’s syndrome (CS) is a rare disorder that can be caused by a number of different problems. The most common cause (65 to 70 percent) is a benign pituitary tumor called an adenoma. Cushing’s syndrome due to a pituitary tumor is sometimes called Cushing’s disease (named after Dr. Harvey Cushing, who provided the initial disease description). The second leading cause of CS is an adrenal tumor (20 to 30 percent), which may be benign or malignant. Lastly, CS can be produced by a variety of cancers originating in other organs due to over secretion of ACTH (10 to 15 percent). This is termed ectopic ACTH.
What are the symptoms of Cushing’s syndrome?
The signs that signal the development of Cushing’s syndrome appear slowly in time. The symptoms are subtle. Some patients may only display a few symptoms while others may have a variety of symptoms. The most noticeable symptom would be a change in physical appearance. The face becomes round, rosy and puffy (the Campbell’s soup girl), there is abdominal weight gain and development of fatty deposits just below the back of the neck. Patients may experience thinning of the skin, with easy bruising and pink or purple stretch marks. Some patients may develop high blood pressure or diabetes. Since cortisol is secreted in response to the normal waking and sleep pattern, patients may experience sleep disturbance. Others may experience rapid emotional changes. Some patients experience a specific type of muscle weakness that makes it difficult to arise from a seated to standing position. Since the signs and symptoms may develop slowly over the course of years, serial photographs of a person’s appearance are often a way to document the changes. Signs of virilization (masculinization) may occur in women.
How is Cushing’s syndrome diagnosed?
Since the signs and symptoms of the disease are subtle and may overlap with other disease processes, a trip to the doctor may be necessary to clarify whether Cushing’s syndrome (CS) is a possibility. The first step to treatment is making the diagnosis. Therefore, the evaluating doctor must recognize CS as the possible cause for the pattern of signs and symptoms. The most widely used test is measurement of the total amount of cortisol contained in a whole day’s urine collection. Medically, this is known as the 24-hour urinary free cortisol test. Another important test is the dexamethasone suppression test where dexamethasone (steroid) pills are given by mouth then blood and urine are collected to assess the levels of cortisol the body. Under normal circumstances, the excessive dexamethasone will suppress the body’s ability to secrete cortisol. In the body of a person with CS, the levels of cortisol will not be suppressed and will remain abnormally high.
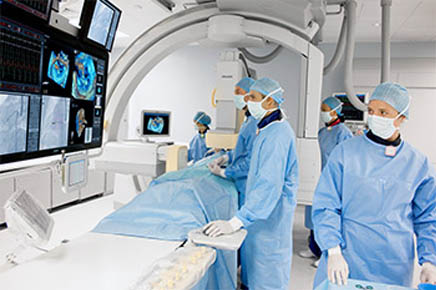
Once the diagnosis of CS is made, then the cause must be identified. This requires the distinction between pituitary tumor, adrenal tumor or ectopic ACTH. A blood test for the determination of both cortitrophin and cortisol taken in the late afternoon is the next step.. When corticotropin is very low or undetectable, it indicates an adrenal tumor. A CT scan or MRI usually confirms the diagnosis. Mildly elevated cortitrophin is associated with pituitary tumors. An MRI of the brain can usually confirm this diagnosis. More sophisticated testing may be needed in some cases when the pituitary tumor is so small that it cannot be seen by conventional imaging techniques. Very high levels of ACTH are associated with the ectopic ACTH syndrome. Testing to look for an underlying tumor should be performed.
How is Cushing’s syndrome treated?
If Cushing’s syndrome is a side effect of taking high doses of prescribed steroid hormones, withdrawing these medicines will allow the body to go back to normal. The ability to reduce or stop the steroids, however, depends on the type of disease being treated and the pattern of response.
Pituitary tumors can be treated with surgery. Usually, an operation can be done through the nose (transsphenoidal surgery). This is performed by a neurosurgeon.
Adrenal tumors can be removed surgically by a urologist. When the adrenal tumor is small (less than six centimeters), the tumor is more likely to be benign. These small tumors can be removed using laparoscopic techniques. Several small cuts are made in the abdomen to pass instruments that dissect and remove the tumor. In less than 5% of operations, the laparoscopic approach may not be feasible and may be converted to an “open” operation. Tumors larger than six centimeters are more likely to be malignant. These tumors are often removed using a larger, open incision. During removal of a large adrenal tumor, adjacent organs such as the spleen, kidney or a portion of the colon may need to be removed to ensure complete tumor removal.
What can be expected after treatment for Cushing’s Syndrome?
Recovery from laparoscopic surgery is rapid. Most patients are discharged within one to two hospital days. Full recovery back to normal activity is three to five weeks. There are usually no physical restrictions after recovery from surgery. It takes longer to recover from open surgery with hospital recuperation between five and 10 days and full recovery taking up to eight weeks.
An important distinction for adrenal tumors is whether or not they are malignant. This is important because the prognosis is very different for benign and malignant tumors. Small adrenal tumors are usually benign and are called adenomas. While size is an important criterion, careful pathologic review of the tumor is the only certain way to determine benign and malignant tumors.
The high levels of cortisol secretion from one adrenal gland suppress the function of the other gland. Postoperatively, patients require supplemental steroids to avoid steroid deficiency. The other adrenal usually recovers, but may take up to a year to do so. In 25 percent of patients, the other adrenal gland never recovers and there may be a need to take steroids as replacement treatment.
Malignant tumors are adrenal cancer. The three-year survival rate is 40 percent and the five-year survival rate is 30 percent. These tumors may recur in the abdominal cavity or spread to the liver, lymph nodes, lungs or bones. Therefore, follow-up CT scans and chest X-rays will be needed at regular intervals if this diagnosis is confirmed. If recurrent disease causes symptoms of Cushing’s syndrome to return, there are drugs that may be used to control this.
Frequently asked questions:
If a person has been diagnosed with Cushing’s syndrome, how normal can they expect their life to be?
The symptoms, disabilities and lifestyle of a person with Cushing’s syndrome (CS) depend on the degree of cortisol excess, the duration of the disease, the basic health of the person and especially the type and curability of the syndrome. If it is cured, all of the features of the disease can subside, but this may take as long as two to 18 months. During that time, most people get annoyed and frustrated by the slow improvements in physical changes. The combination of CS and adrenal insufficiency signs and symptoms (e.g., dizziness, weakness, nausea and loss of appetite) decrease as replacement steroid hormones are tapered and adrenal hormone production slowly improves toward normal. Frequent calls and visits to a physician are necessary.
If the CS is incurable, or if medically-induced CS remains, these individuals will have to cope with persistent fatigue, muscle weakness, abdominal and facial weight gain, depression, mood swings and all the other signs and symptoms mentioned earlier. Drugs are available to moderate these residual symptoms. Regular visits to a physician for examinations, blood tests and treatments of infections and complications will be necessary and are often viewed as a severe burden.
What is the difference between Cushing’s syndrome and Cushing’s disease?
Any condition that causes the adrenal gland to produce excessive cortisol results in the disorder known as Cushing’s syndrome (CS). CS is characterized by facial and torso obesity, high blood pressure, stretch marks on the belly, weakness, osteoporosis and facial hair growth in females.
CS has many possible causes, including tumors within the adrenal gland, ectopic cortitrophin produced from cancer such as lung cancer and cortotrophin excessively produced from a pituitary tumor within the brain. Corticotrophin is normally produced by the pituitary gland (located in the center of the brain) to stimulate the adrenal glands’ natural production of cortisol, especially in times of stress.
When a pituitary tumor secretes excessive cortitrophin the disorder resulting from this specific form of CS is referred to as Cushing’s disease.
As an aside, it should be noted that doctors sometimes describe certain patients with features identical to CS as having “Cushingoid” features. Typically, these features are occurring as side effects of cortisone-related medications, such as prednisone and prednisolone.
Can stress cause Cushing’s syndrome?
Stress-related increased cortisol production by the adrenal glands is normal and physiological, and does not lead to Cushing’s syndrome.


Good post. I’m experiencing many of these issues as well..
Hi there
Would you like to easily see a birds eye view of what your current and past customers think about you? Do you know what people are saying about you? Whether its hurting or helping your business?
My name is Paul, the Outreach Director of Five Star Fast Lane, and for the price of, well, nothing –I would like to provide you with a full detailed report on your current business standings. As a bonus, our report scanner will report back with any inaccuracies about your business that are out there potentially causing you loss of revenue and customers.
There is no obligation or a catch, the report is yours to use as you see fit. Feel free to make use of it.
Regards
Paul
Five Star Fast Lane
PS – If you want to discuss the results we are available via live chat daily on the site.
Good site! I really love how it is easy on my eyes and the data are
well written. I’m wondering how I could be notified when a new post has been made.
I’ve subscribed to your RSS which must do the trick!
Have a nice day!