There are many reasons why a person can have blood in their urine. This condition, known as hematuria, can be an indication of a serious problem or conversely, have no negative connotation. What should you do if you find out that there’s blood in your urine? Read the following to learn more.
What is hematuria?
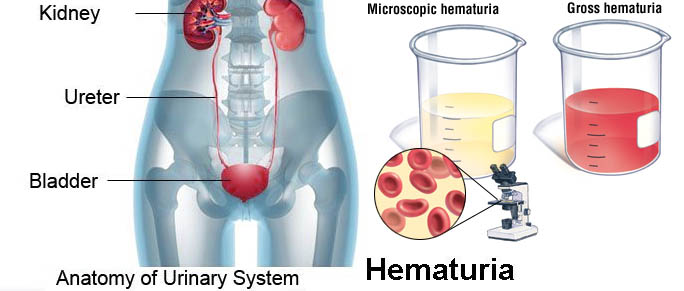
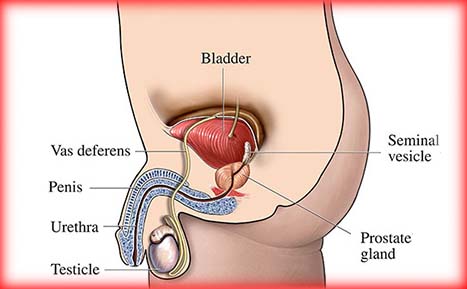
Hematuria is defined as the presence of red blood cells in the urine. It can be characterized as either “gross” (visible to the naked eye) or “microscopic” (visible only under the microscope). Microscopic hematuria is an incidental finding often discovered on urine tests as part of a routine medical evaluation, whereas gross hematuria could prompt you to visit the doctor. Hematuria can originate from any site along the urinary tract, including the kidneys, ureters, bladder, prostate and urethra. It is estimated that hematuria occurs in 2.5 to 21 percent of the population. In many patients no specific cause is found; however, hematuria may be a marker for infection, stone disease or urinary tract cancer. Risk factors for significant underlying disease include: smoking, radiation, overuse of some pain medicines and exposure to certain chemicals.
What are the common causes of hematuria?
Blood in the urine is often not a sign of significant disease. Studies have shown that between nine to 18 percent of normal individuals can have some degree of hematuria. However, hematuria can be a sign of an important medical condition requiring treatment. Below is a list of common causes of hematuria:
- Bladder Cancer
- Kidney Cancer
- Prostate Cancer
- Ureteral Cancer
- Urethral Cancer
- Urinary Stone Disease
- Urinary Tract Infection
- Pyelonephritis (Kidney Infection)
- Benign Prostatic Hypertrophy (Enlarged Prostate)
- Renal (Kidney) Disease
- Radiation or Chemical Induced Cystitis (Bladder Irritation)
- Injury to the Urinary Tract
- Prostatitis (Prostate Infection)
- Exercise Hematuria
How is hematuria diagnosed?
Visible hematuria is often worrisome to the patient and prompts them to seek medical attention; however, microscopic hematuria can be just as severe. It often has no symptoms and is detected on a urine dipstick test. If the dipstick test is positive for blood the amount of blood is often determined by looking at the urine with a microscope. If three or more red blood cells (RBC) are seen per high power field on two of three specimens, further evaluation to determine a cause is recommended.
What additional tests are needed?
Any patient with gross hematuria or significant microscopic hematuria should have further evaluation of the urinary tract. The first step is a careful history and physical examination. Laboratory analysis consists of a urinalysis and examination of urinary sediment under a microscope. The urine should be evaluated for protein (a sign of kidney disease) and evidence of urinary tract infection. The number of red blood cells per high-powered field should be determined. In addition the shape of the blood cells should be evaluated. This can help determine where the bleeding is coming from. In patients with white blood cells in the urine, a urine culture should be performed as well. A urinary cytology is also obtained to look for abnormal cells in the urine. A blood test should also be done to measure serum creatinine (a measure of kidney function). Those patients with significant protein in their urine, abnormally shaped red blood cells, or an elevated creatinine level should undergo general medical evaluation for the presence of kidney disease.
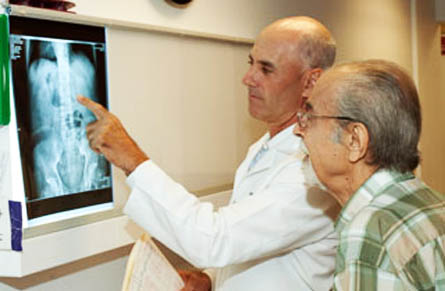
A complete urologic evaluation for hematuria also includes X-rays of the kidneys and ureters to detect kidney masses, tumors of the ureters and the presence of urinary stones. This traditionally consisted of an intravenous pyelogram (IVP). In this study, a radiographic dye is injected into the blood stream and X-rays are taken as the kidneys excrete the dye. This study has trouble detecting small renal masses and is often combined with a renal ultrasound.
Many physicians may opt for other imaging studies such as a computerized tomography (CT) scan. This is the preferred method of evaluating kidney masses and is the best modality for the evaluation of urinary stones. Recently many urologists have been using CT urography. This allows the urologist to look at the kidneys and ureters with one X-ray test. In patients with an elevated creatinine or an allergy to X-ray dye, magnetic resonance imaging (MRI) or retrograde pyelography is used to evaluate the upper urinary tract. During retrograde pyelography, the patient is taken to the operating room and dye is injected up the ureters from the bladder and then images are taken.
The main limitation of these imaging studies is the inability to evaluate the bladder; therefore a cystoscopic evaluation is required. This is usually performed in the office under local anesthesia with either a rigid, or more commonly, a flexible cystoscope. After applying a topical analgesic to the urethra the urologist inserts an instrument called a cystoscope through the urethra and into the bladder. Looking through the cystoscope the doctor can examine the inner lining of the bladder and urethra for abnormalities.
What happens if no abnormality is found?
In at least eight to 10 percent of cases no cause for hematuria is found. Some studies have demonstrated an even higher percentage of patients have no cause. Unfortunately, studies have shown that urologic malignancy is later discovered in one to three percent of patients with negative work-ups. Therefore, some form of follow-up is recommended. Recommendations regarding follow-up are sparse and no clear consensus has been agreed upon. Consideration should be given to repeating the urinalysis and urine cytology at six, 12, 24 and 36 months. Immediate re-evaluation with possible cystoscopy and repeat imaging should be performed in the face of gross hematuria, abnormal urinary cytology or irritating urinary symptoms such as pain with urination or increased frequency of urination. If none of these symptoms occur within three years, no further urologic testing is needed.
How will hematuria be treated?
Treatment will be based on a physician’s evaluation of the patient’s condition, symptoms and medical history along with the cause of the hematuria.


Keep these artlcies coming as they’ve opened many new doors for me.
Excellent blog here! Also your site loads up
very fast! What host are you using? Can I get your affiliate link
to your host? I wish my web site loaded up as quickly as
yours lol