Regular Pap tests and pelvic examination help prevent cervical cancer, finds Dr Parul R Sheth
CANCER of the cervix holds the top position on the list of cancers in women. The good news, however, is that there are ways to prevent cervical cancer by getting Pap tests and pelvic exams done regularly. Your doctor can find and treat the changing cells before they turn into cancer.
Reveals Dr. Dharma R Choudhary, Senior Consultant & Director – BLK Super Speciality Hospital, Delhi for Bone Marrow Transplant, “An estimated number of 4,70,000 new cases of cervix cancer are diagnosed each year worldwide. Over 80 per cent of the cases occur in developing countries, where in many regions, it is the most common cancer among women. Around 27 per cent of the cases occur in India from where 1,26,000 new cases are diagnosed annually and over 71,000 deaths due to cervix cancer are reported each year. Over 60 per cent of the cases report for treatment in fairly advanced stages of the disease.”
WHAT CAUSES IT?
“We do not know exactly what causes cervical cancer, but certain risk factors are believed to have an effect.The most significant risk factors are Human Papilloma Virus (HPV) and sexual history. Specific types of HPV (the same virus that causes genital warts) are linked with 95 per cent of cases of cervical cancer. HPV is passed on through sex and usually causes no symptoms at all. A woman has a higher-than-average risk of developing cervical cancer if she starts to have sex at an early age (<18 years) and may expose the cervix to HPV at an especially susceptible time. Plus, the more sexual partners a woman has, the greater the risk of getting HPV,”says Dr. Rahul Bhargava.
“Cervical cancer is a sexually transmitted disease and it occurs more commonly in women who marry early, have children at an early age or have multiple pregnancies, or are infected with HIV,”adds Dr. Vinod Raina, professor and head of the Genito Uro Oncology services at the BLK Super Speciality Hospital, Delhi. In addition, says Dr Bhargava,“Various other risk factors have also been identified – tobacco use, poverty, hormonal medications (birth control pills) taken for long periods of time, women with weakened immune system, especially those who are HIV positive, or women with a history of abnormal cells (dyskaryosis).”
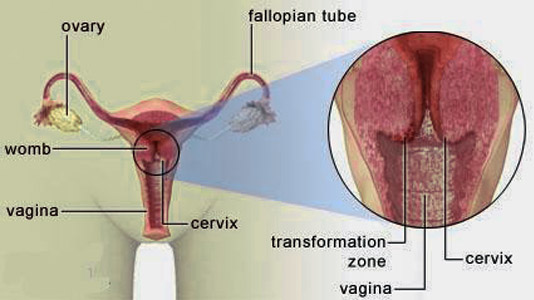
The mucus-producing lining of the cervical canal (called “columnar” tissue after the shape of its outer cells) meets the surface covering of the vagina (made up of squamous epithelial cells) at a line of demarcation called the “squamocolumnar junction.” It is in this shifting zone of disparate cells that abnormal growth is most likely to arise. Central to the Pap test is an adequate sample from this point.
CHANGES IN THE CELLS
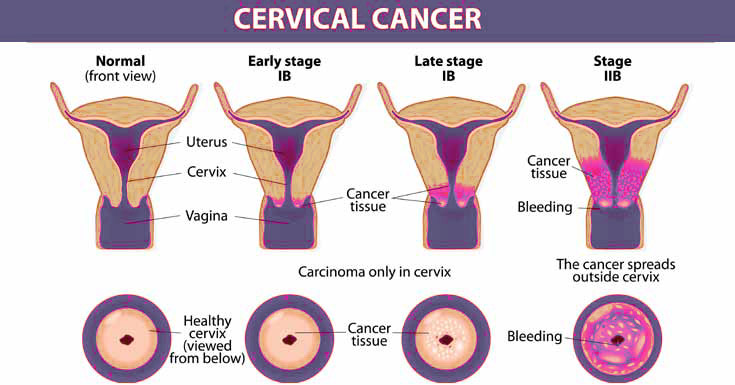
The cells in the outer layer of the cervix, the entrance to the uterus, located at the top of the vagina begin to show abnormal microscopic changes.This stage is called dysplasia.“Dysplasia,”says Dr Raina,“Is found in women between the ages of 25-35 years.The cells to grow from normal to dysplasia stage to cancerous cells takes around 15 years but once the cancer becomes invasive, it spreads quickly.”According to Dr Bhargava, cervical dysplasia is an important health problem because it sometimes, but not always, progresses to cervical cancer.
Once the cancer moves beyond the outer layer of the cervix, it invades the uterus, the vagina, bladder and rectum.
SYMPTOMS
Says Dr Raina,“Generally, cervical cancer afflicts women after 40 years of age. In its early stages it does not cause any symptoms. However, inter-menstrual bleeding, bleeding following intercourse or postmenopausal bleeding, vaginal discharge – may indicate a presence of malignancy. Unfortunately, 70 per cent of women come to us in advanced stage of cervical cancer.”
AT THE DOCTOR’S CLINIC
The tests begin with a pelvic exam.The doctor then does a Pap test. Says Dr. Esha Kaul, Prof. Medical Oncology/ Haematology and Director-Oncology, Jaypee Hospital, Noida,“If the test shows irregularly shaped cells (dysplasia) or cancer cells, the doctor will further examine your cervix using a colposcope and do a biopsy (remove a small piece of tissue) for further check and CT scan if necessary.”Endocervical curettage or endocervical scraping may also be done.
DNA testing also can be done to check for the presence of HPV infection in cervical secretions, and to determine the type of HPV. Some HPV types are more likely to cause cancer.
Dos and Don’ts
- Avoid multiple sex partners
- Practice safe sex. Use condoms
- Stop smoking
- Maintain good genital hygiene
TREATING CERVICAL CANCER
The treatment depends upon the stage of the cancer. If you are in your early stages and are pregnant, the doctor may postpone the treatment until after delivery. “In selected patients – usually those who are older and have no desire for future pregnancy”says Dr Bhargava,“The doctor may recommend a hysterectomy to treat severe cervical dysplasia. This is especially true if the patient already has significant uterine problems, such as fibroids or abnormal uterine bleeding.”
“For women who are young and wanting to have children, procedures such as laser surgery, in which the superficial tissue layer is heated and vaporised, cryosurgery, in which the tissue to be removed is frozen, conization, surgical removal of a cone of cervical tissue or loop electrosurgical excision procedure (LEEP) are used as treatment procedures,”informs Dr Raina.
“Chemotherapy and/or radiation is reserved only for patients who have frank cancer. It is not recommended for patients with dyslpasia alone,”states Dr Kalra. The cure rates according to Dr Raina are 85 per cent in the early stages (stage 1), 65-75 per cent in stage 2 and about 45-50 per cent in stage 3 cancers.
Says Dr Bhargava,“Newer experimental treatments are also being used to treat cervical dysplasia with vitamin A derivatives called retinoids, but so far these have not been more effective than standard therapies.”
FOLLOW-UP IS A MUST
“The patient is usually followed closely for 8-10 years to confirm that cervical dysplasia does not return. During this follow-up period, the patient’s doctor may recommend a diet rich in carotene, vitamin C, vitamin E and folic acid, since there is some evidence that these nutrients may offer some protection against cervical cancer,”states Dr Bhargava.
According to Dr Kaul,“Clinical exam is necessary as a follow-up after surgery for cervical cancer, to see whether there is any recurrence.”Says Dr Kalra,“Pap smear is not recommended for follow up in a patient who has already been diagnosed as having cancer or has undergone treatment for cancer. In these circumstances, the tests required for follow up are different.”
PREVENTION IS BETTER THAN CURE
Dr Dua advises,“One should maintain safe sex (barrier contraceptives like condoms), good genital hygiene, and get Pap smear done once in three-five years for women over 30 years.”Detecting cervical cancer early dramatically increases your chances of survival.“It is a must that women should get Pap smear done on a regular basis for it can tell three years in advance about the occurrence of cancer, avoid multiple partners and multiple pregnancies too,” stresses Dr Kaul.
Test in time
Cervical cancer is a totally preventable disease and yet women die of cervical cancer every year in developing countries. A majority of them die because they have never had a cervical smear.
A cervical smear (also called a Pap test or Papanicolaou smear) is a simple and a quick screening test for cervical cancer and for the early cell changes which may eventually lead to cervical cancer.
Describes Dr. Manas Kalra, Professor and Head of Medical Oncology, Apollo Hospitals, Indraprastha, New Delhi, “The woman is made to lie down on an examination table.The cervix area is visualised (using a special position) and a sterile wooden or plastic disposable devise (spatula) is rotated around the surface of the woman’s cervix (on the cervical os).
This results in surface cells from the cervix sticking on to the wooden device. These cells are then fixed in a chemical solution, stained and examined by a cytologist under the microscope. From the appearance (morphology) of these cells the specialist can make out whether the cells are normal, abnormal (displastic) or frankly cancerous.”
Says Dr. Vikas Dua, Head of the Department, Preventive Oncology, Fortis Memorial Research Institute, Gurgaon, “The test when done in places like the Fortis Hospital where good quality standards are maintained the test has a sensitivity around 80 per cent and a specificity around 95 per cent. It is essentially a good screening test and cervix cancer incidence and mortality rates have been reduced significantly in the developed countries where Pap smear screening is routinely practiced.”
However, according to Dr Kalra, “Pap smear is very expensive and requires specialists to evaluate the slides.This is not cost effective for routine screenings. Alternate screening tests are available – including VILI and VIA.These are more applicable in developing countries.”
The mucus-producing lining of the cervical canal (called “columnar” tissue after the shape of its outer cells) meets the surface covering of the vagina (made up of squamous epithelial cells) at a line of demarcation called the “squamocolumnar junction.” It is in this shifting zone of disparate cells that abnormal growth is most likely to arise. Central to the Pap test is an adequate sample from this point.